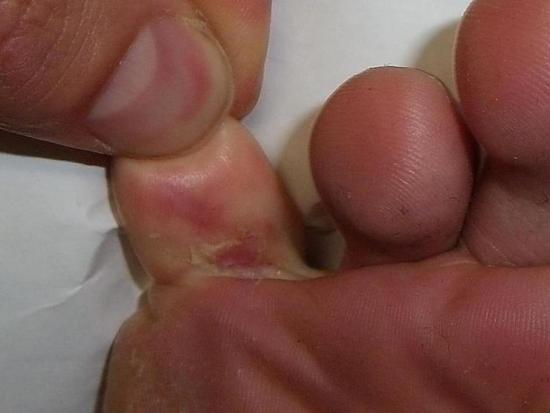
An athlete’s foot infection is a fungal infection that affects the upper layer of the skin of the foot, particularly whenever the foot is warm, damp, and inflamed.
Tinea pedis and ringworm of the foot are other names for this condition. Trichophyton is the fungus that causes athlete’s foot. It can be found on floors and in clothing.
Conditions for athlete’s foot fungal infection are critical – it has to be in a warm, moist environment, such as the inside of a shoe, in order to cause inflammation of the skin. As a result, only about 0.75 percent of those who walk barefoot on a regular basis are affected.
Athletes’ foot, on the other hand, can affect up to 70% of the population at some point in time.
The most typical location for athlete’s foot to form is between the toes. It is commonly associated with burning, stinging, redness, and itching. Some patients experience flaking of the skin as a side effect of this medication.
It’s the most common kind of fungus. Athlete’s foot can be treated using over-the-counter (OTC) medications, despite the fact that it is contagious in nature. Individuals with a weaker immune system or diabetes, on the other hand, should seek medical attention as soon as athlete’s foot appears.
Causes
Trichophyton, the fungus that causes athlete’s foot, is a dermatophyte which means it is linked to other fungi that cause infections in the skin, hair, and nails of humans.
These fungus can be found on the surface of human skin and are completely harmless. As long as the skin is dry and clean, their ability to reproduce is severely restricted. They do, however, multiply fast when exposed to moist and warm circumstances.
It is more likely that thick, tight shoes will develop athlete’s foot because they push the toes together, producing an ideal environment for the fungal infection to grow. The use of plastic shoes, which are known to warm and wet the feet the most, is associated with a greater risk of athlete’s foot than the use of other materials such as leather or canvas, according to experts.
If the socks are wet and the feet are heated, the likelihood of acquiring athlete’s foot increases significantly.
An athlete’s foot infection can spread by direct and indirect contact with the affected area:
- direct, skin-to-skin contact, as may occur when an uninfected person touches the infected area of somebody with athlete’s foot
- indirect contact, in which the fungi can infect people via contaminated surfaces, clothing, socks, shoes, bed sheets, and towels
Athlete’s foot is most typically found in swimming pools and community showers, which are both humid and warm environments.
The possibility of developing athlete’s foot is increased in people who have compromised immune systems.
Symptoms
The skin on the foot, particularly between the toes, becomes irritable; there is also a sensation of stinging or burning in the affected area. It is also possible for the skin to become:
- dry
- flaky
- red
- scaly
- cracking
It is possible that the skin will crack, and there will be oozing or crusting, as well as irritating blisters and swelling. Scaling patterns may appear on the sole of the foot as well as the sides of the foot.
Bacterial infections can arise in conjunction with the disease in sometimes. When athlete’s foot is severe and results in open sores on the skin, the skin becomes more sensitive to infection of bacteria.
If the infection is not treated immediately, there is a chance that it will spread from toe to toe. It is possible that a rash will develop on the sides and bottoms of the feet. Tinea manuum is the term used to describe athlete’s foot that has migrated to the hands in rare circumstances. In many ways, the symptoms are comparable to those that are experienced by people with foot problems.
People who do not wash their hands quickly after contacting the afflicted region on their foot are at greater risk of contracting the infection. An athlete’s foot complication called tinea manuum is extremely rare.
If the patient scratches the infected region and then touches other parts of his or her body, the infection has a chance of spreading further. It is critical to treat athlete’s foot as soon as the first signs of the condition arise. It is critical to properly wash hands with soap and warm water after coming into contact with the infected region.
Pictures
Diagnosis
Athlete’s foot may usually be identified by looking at the characteristic signs and symptoms of the condition. A doctor, on the other hand, may wish to rule out other conditions such as dermatitis, psoriasis, or a low-grade skin infection before making a diagnosis.
The skin lesion potassium hydroxide test is the most commonly used. An infected tissue sample is taken and placed in a solution of potassium hydroxide (KOH) by the doctor during this test. Human cells are destroyed by the KOH solution, leaving only the fungus cells behind. A microscope can be used to examine these specimens.
Treatments

Fortunately, in the vast majority of cases, athlete’s foot symptoms are moderate, and the patient does not require medical attention.
OTC drugs, which are available at pharmacies and are successful in clearing up the infection, can be purchased.
Occasionally, a doctor may prescribe a stronger antifungal medicine, which is usually swallowed, in more severe situations.
These medications work by killing the fungus that is causing the symptoms. Antifungal medicines are offered in the following forms:
- tablets
- powders
- liquids
- sprays
- creams
The majority of topical drugs are available over-the-counter. Topical refers to something that is applied directly to the skin. If you have fungal infections, your pharmacist may recommend one of the following antifungal medications:
- clotrimazole
- econazole
- ketoconazole
- miconazole
- terbinafine
- sulconazole
These oral treatments may be administered by a doctor if the symptoms are severe or if the topical medications have failed to provide relief:
- griseofulvin
- itraconazole
- terbinafine
Antacids have been shown to interfere with the absorption of oral antifungal medications. Oral antifungals may potentially have an impact on the way some anticoagulant medications work.
Some forms of antifungals should not be administered to elderly individuals or children under the age of 6. Consult with a pharmacist, doctor, or nurse, or carefully read the patient information booklet that comes with the drug.
Children may require different dosages than adults. Some drugs are processed by the liver, and blood tests may be required to ensure that the patient’s liver is in good health before the prescription can be prescribed.
Some antifungals should not be taken during pregnancy, while others may have an adverse effect on both the male and female reproductive systems if taken during pregnancy. Individuals who are pregnant or who intend to become pregnant should consult with a medical professional.
Hydrocortisone
It is possible that the doctor will prescribe hydrocortisone if the skin becomes extremely painful and there is a lot of edema. Low-dose hydrocortisone medicines can be purchased over-the-counter – greater dosages would necessitate a physician’s prescription.
Antacids have been shown to interfere with the absorption of oral antifungal medications. Oral antifungals may potentially have an impact on the way some anticoagulant medications work.
Some forms of antifungals should not be administered to elderly individuals or children under the age of 6. Consult with a pharmacist, doctor, or nurse, or carefully read the patient information booklet that comes with the drug.
Children may require different dosages than adults. Some drugs are processed by the liver, and blood tests may be required to ensure that the patient’s liver is in good health before the prescription can be prescribed.
Some antifungals should not be taken during pregnancy, while others may have an adverse effect on both the male and female reproductive systems if taken during pregnancy. Individuals who are pregnant or who intend to become pregnant should consult with a medical professional.
Hydrocortisone
It is possible that the doctor will prescribe hydrocortisone if the skin becomes extremely painful and there is a lot of edema. Low-dose hydrocortisone medicines can be purchased over-the-counter – greater dosages would necessitate a physician’s prescription.
Home remedies
Steps can be taken at home
- Wash feet often with soap and water
- Soak feet in salt water or diluted vinegar to clear up blisters
- Some evidence shows that soaking feet in a tea tree oil solution can help. Tea tree oil can be purchased online.
- Make sure feet are completely dry after washing, especially between the toes
- Wear clean cotton socks
- To keep feet dry, change shoes and socks often
- Wash towels regularly, do not share them
Prevention
The key to reducing the danger of acquiring athlete’s foot is to keep your feet, shoes, and socks clean and dry at all times.
Experts advise the following:
- Wash the feet twice a day with water and soap. Always clean between the toes.
- Keep feet dry. Applying antifungal talcum powder to the feet can help. Walk barefoot at home as much as possible.
- Remove shoes as soon as exercise or sports has ended.
- Wear loose-fitting, well-ventilated shoes, especially during the warmer months. The best materials for shoes are leather or canvas.
- Make sure feet are dry before putting on socks, stockings, or tights. Wear socks made from material that draws moisture away from the feet, such as cotton, silk, or wool.
- When walking around public swimming pools and communal changing rooms and shower areas, wear pool slippers.
- Change shoes regularly so that footwear is relatively dry. Shoes need time to dry out.
- Do not share footwear.
- Wash sheets and towels regularly.
- If a pet in the home has hair loss, this could be a sign of athlete’s foot – take it to the vet. Humans can catch athlete’s foot from their pets.
Children who have athlete’s foot can still attend school, but the instructor should be informed so that proper precautions can be taken before and during physical education lessons. While in school, the child should not be allowed to walk barefoot.
Complications
Despite the fact that athlete’s foot symptoms are often moderate and consequences are infrequent, professionals advise treating the condition as soon as possible. Complications are considerably reduced when treatment is initiated as soon as possible.
Fungal nail infection: Undiagnosed athlete’s foot can extended to toenails in a condition called as onychomycosis. The nail gets thick, opaque, whitish, and crumbly as the condition progresses. It is possible that there will be discomfort and inflammation in the skin beneath the nail. If left untreated, toenail infections can progress to the point where they cause additional discomfort and make it difficult to wear shoes or even walk.
Secondary bacterial infection: Eventually, the foot may become painful, heated, and swollen as a result of this development.
Infected lymph system: In some cases, the infection might extend to the lymphatic system. It is important to note that lymphangitis is an infection of the lymph vessels, while lymphadenitis is an infection of the lymph nodes.
Cellulitis: This is a bacterial infection that has penetrated deep into the skin. Skin, fat, and soft tissue are all possible sites of involvement. Septicemia (blood poisoning) and bone infection are both possible outcomes if cellulitis is left untreated for an extended period of time. Cellulitis is a relatively unusual complication of athlete’s foot that should be treated as soon as possible with antibiotics.
Allergy: The fungus that causes athlete’s foot can produce allergic reactions in certain people, which can result in blistering on the hands or feet.
Sources
- http://onlinelibrary.wiley.com/doi/10.1046/j.1440-0960.2002.00590.x/abstract
- http://www.acfaom.org/information-for-patients/common-conditions/athletes-foot
- http://www.nhs.uk/conditions/Athletes-foot/Pages/Introduction.aspx
- https://www.medicalnewstoday.com/articles/261244
- http://www.aafp.org/afp/2003/0101/p101.html
- http://www.mayoclinic.org/diseases-conditions/athletes-foot/diagnosis-treatment/diagnosis/dxc-20235949
- http://www.mayoclinic.org/diseases-conditions/athletes-foot/symptoms-causes/dxc-20235876
- http://www.cdc.gov/fungal/diseases/ringworm/treatment.html