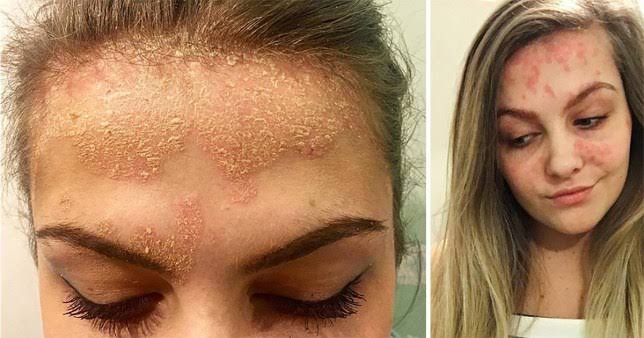
There is an increasing number of injectable medications available to treat psoriasis, a disease in which a person develops excess skin cells on their body, leading to changes in the skin and other symptoms.
Scientists don’t know exactly what causes psoriasis, but they suspect it occurs when healthy cells are damaged by the immune system, causing skin cells to grow too quickly.
Psoriasis is a persistent ailment. There is no cure at the moment, but medicine can help control symptoms and new treatments for certain types of psoriasis are becoming more effective than previous ones.
People have historically used over- the-counter treatments, lifestyle remedies, and certain prescription drugs to treat psoriasis, but physicians may now prescribe injectable drugs known as biologics for some forms when the symptoms are moderate to severe.
In recent years, a number of new medications have been approved by the Food and Drug Administration (FDA), and there is hope that these can greatly improve the quality of life for psoriasis sufferers.
As with all drugs, there are possible side effects. Before a medicine is administered a doctor may discuss these with the patient.
Biologics
Most of the injectable psoriasis prescription drugs are known as biologics drugs, or “biologics,” which target the immune system.
Different biologics work in different ways but all target cytokines, a type of protein produced by the immune system.
Cytokines play a role in defending the body against harmful or unwanted substances under normal circumstances. Inflammation occurs when the body produces extra cytokines as part of its immune response. This usually happens but in some cases, including psoriasis, the immune response persists and the inflammation continues.
Scientists make the biologics they create in a laboratory from living cells. They extract specific protein forms from these cells, and use them in drugs. Such drugs help to relieve psoriasis symptoms by reducing the extra immune response involved in psoriasis.
Multiple drugs approved by the FDA to treat psoriasis.
Some of those medicines in the immune system can target special T-cells. Others can stop the growth of proteins inside the immune system.
Doctors usually only prescribe these medicines when a person has a mild to severe psoriasis, and other therapies have not worked.
Interleukin-12 and -23
Two of the proteins that the body produces as part of the immune response are interleukin-12 (IL-12) and interleukin-23 (IL-23). These are all related to signs of psoriasis. Blocking such protein’s activities will reduce inflammation of psoriasis.
Ustekinumab (stelara) is an IL-12 blocker with FDA approval for treating different types of psoriasis. It binds to bothIL-12andIL-23, and reduces their body effects.
The FDA has also approved IL-23 antagonists for the treatment of plaque and other types of psoriasis:
- Guselkumab (Tremfya)
- Tildrakizumab (Ilumya)
- Risankizumab (Skyrizi)
Risankizumab is currently awaiting FDA approval.
Interleukin-17A
IL-17A is another protein that seems to cause a psoriasis-causing reaction in the immune system. It may also prevent the reaction from preventing this action.
Examples of psoriasis injections approved by FDA which block IL-17A include:
- secukinumab (Cosentyx)
- ixekizumab (Taltz)
- brodalumab (Siliq)
Tumor necrosis factor-alpha blockers
Cytokine proteins can cause inflammation in the body. One form of cytokine is the tumor necrosis factor-alpha (TNF-alpha).
When a person is suffering from a condition such as rheumatoid arthritis or psoriasis, too much TNF-alpha is released. Blocking the development of TNF-alpha would, in principle, avoid some symptoms of psoriasis.
The following TNF-alpha blockers have been licensed by the FDA to treat psoriasis:
- adalimumab (Humira)
- certolizumab pegol (Cimzia)
- etanercept (Enbrel)
- golimumab (Simponi)
- infliximab (Remicade)
A doctor should administer Remicade instead of a regular injection, using an intravenous (IV) infusion.
The doctor will speak to the patient about the available medications, how they can be used and the possible side effects. They will choose a medication that fits the type of psoriasis the patient has.
We should also track the individual to check for any unwanted effects and if one choice appears to be inappropriate we may suggest an alternative.
Methotrexate
Another drug-methotrexate (Trexall, Rheumatrex)-may be prescribed by a doctor to treat psoriasis. Methotrexate is a systemic medicament. This means it works all over the body— like the biologics— but it’s not a biologic.
Instead, it is an anti-rheumatic medication the modifies the disorder, or DMARD. It works to suppress the immune system, but this is done differently than the biologics.
In addition to a biological or other treatment, a doctor can prescribe this drug. The combination needs FDA approval, because it may increase the risk of adverse effects by combining certain medications.
Methotrexate is available either in pill form as an oral drug or as an injection.
Methotrexate may have certain side effects. Drugs which reduce the immune system’s action may increase the risk of infections. Studies have shown that this risk may be increased by combining methotrexate with other medications.
Physicians initially recommended methotrexate as a chemotherapy agent for treating cancer in greater dosages. Today, a variety of health conditions, including psoriasis and rheumatoid arthritis, are treated with it.
Benefits and drawbacks
Injectable drugs prove effective in reducing the effects of moderate to severe psoriasis symptoms.
Injections of TNF-alpha blockers may also aid in patients with psoriatic arthritis to minimize long-term joint damage.
The frequency at which an individual needs an injection will range from twice a week to once every three months.
The individual will have to go to the doctor’s office each time for some of these treatments. They can learn how to use this at home for others.
It may be inconvenient to see the doctor regularly for an injection but it also helps the doctor to monitor the symptoms and test for any adverse drug reactions.
Risks
Drugs can impact the immune system can have severe side effects.
They can leave someone more vulnerable to infections like tuberculosis (TB).
Before and during treatment, a doctor will screen a patient for TB.
It remains unclear how biological drugs affect pregnancy. It is for this reason that physicians seldom recommend them for pregnant or nursing women.
Side effects of psoriasis injections can range from mild to severe.
Adverse effects of biologic drugs
More common side effects include:
- a higher risk for respiratory or urinary tract infections
- headaches
- flu-like symptoms, such as low energy and body aches
- reactions at the injection site, such as redness, swelling, or discomfort
Rarer side effects include:
- blood disorders
- a higher risk of certain cancer types
- an increased risk of serious nervous system disorders, including multiple sclerosis (MS), nervous system inflammation, and seizures
Adverse effects of methotrexate
Methotrexate is not a synthetic drug, and its side effects are different. The most popular are:
- nausea
- appetite loss
- fatigue
Long-term methotrexate treatment can lead to:
- liver damage
- changes to red and white blood cell production
A doctor will warn a person receiving psoriasis injections about the possible side effects and symptoms they may have. Anyone who develops symptoms that are unfamiliar or worsening after taking a drug should contact their doctor.
Other treatment options
There are several different types of psoriasis, so different approaches might be required.
When prescribing a treatment a doctor will consider:
- the psoriasis type
- where the symptoms are
- how severe the symptoms are
Topical treatments
Many people use topical treatments to remedy the external symptoms of psoriasis.
Topical corticosteroids can reduce inflammation in the skin in cases of mild to moderate psoriasis.
Long-term use of steroids may however contribute to side effects, including an increased risk of cataracts and osteoporosis.
Other treatments include:
- oral and topical vitamin D analogues
- anthralin (Dritho-Scalp)
- calcineurin inhibitors, such as tacrolimus (Prograf)
- salicylic acid
- coal tar
- moisturizers
- topical retinoids, such as tazarotene (Tazorac, Avage)
Additional medication options
Intestinal corticosteroids, retinoids, and cyclosporine are other intestinal therapies.
Oral corticosteroids are a systemic treatment capable of improving symptoms across the body. Treatment with steroids can have side effects. These may involve rebound psoriasis or a triggering of a more serious form of the disease but how this impacts remain unclear to a person with psoriasis, according to a 2012 report.
Retinoids (Soriatine, acitretin) are a form of vitamin A . They come in oral or topical form. They can help some people, but seeing the effects may take several months.
Cyclosporine is an immune suppressant people are allowed to take as a daily pill. Many people could benefit from that. The doctor will have to monitor the blood pressure and health of the person’s kidney.
Apremilast (Otezla) is a DMARD which can minimize psoriasis plaque incidence. It can be taken by people by hand. The authors of a study described it as “well tolerated” in 2017. To monitoring adverse effects, the user does not need ongoing laboratory testing.
Apremilast: is an inhibitor of Phosphodiesterase 4 (PDE4). Research has found linkages between PDE4 and the inflammation that contributes to psoriasis, and taking a PDE4 inhibitor may help lower the occurrence of plaques with psoriasis.
Home remedies
Light therapy could help. Which include exposing the skin to some amount of UV light, usually in a doctor’s office.
Excess UV-light exposure will increase the risk of skin cancer. At least one study concluded that a person with psoriasis may benefit from sun exposure, but they need to do this slowly and carefully because too much sun will aggravate the symptoms.
People living in an area with little access to sunlight should ask their doctor about using an artificial light source, like a light box.
Lifestyle changes
Psoriasis is a skin condition which is inflammatory. Some lifestyle choices may cause inflammation, and may intensify psoriasis symptoms.
Examples might include:
- stress
- smoking
- intense or prolonged sun exposure
Such factors may not cause symptoms in everyone with psoriasis but they may find their symptoms improved if a person cuts them out.
Alcohol can have an effect on how well psoriasis medications function, so avoiding alcohol can benefit some.
Home remedies
Lukewarm water bathing can help, particularly if one of the following is added to the water:
- unscented bath oil
- colloidal oatmeal
- Dead Sea salts
- Epsom salts
Applying moisturizers to the skin may also be helpful after taking a bath.
When to see a doctor
Someone taking treatment for injectable psoriasis will contact their doctor if there are signs of an infection there. This can get worse quickly and be more difficult to treat if the person’s treatment affects their immune system.
The Infection Signs include:
- fever
- cough
- flu-like symptoms
- sores that do not heal
Also, the person should see their doctor if they have any symptoms or side effects of a medication, or if their symptoms get worse. Often, after a while, a biologic gets less powerful. The doctor may need to change the dosage, or recommend another drug.
Takeaway
Biologic and other injectable medications may be successful in the treatment of serious to moderate psoriasis, though side effects may sometimes occur.
A person sh ould discuss their prescription with their doctor, and should inform the doctor if any adjustments or problems arise.