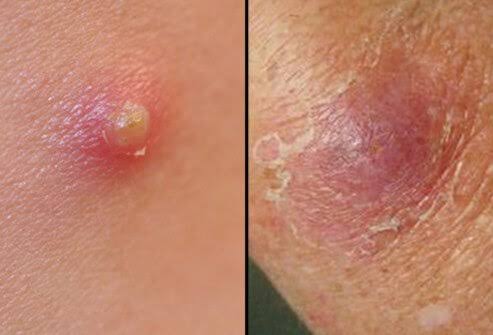
A skin infection caused by Staphylococcus aureus bacteria is a boil or furuncle. In warm, moist skin areas, most commonly the nostrils, armpits, the crease between the buttocks, and the inner thighs, it appears to thrive.
Boils will spread underneath the skin and cluster as well. If this occurs, deeper abscesses called carbuncles are produced by the clusters, which can scar the skin.
Depending on how serious it is, or the amount of skin involved, the size and color of a boil can vary. Many boils seem to have a similar appearance, however.
Important facts about boils
Fast facts about boils on the inner thigh:
- Normally, boils are not a cause for concern and do not require medical attention.
- It is usually not safe to drain boils at home.
- There are many ways to prevent boils from forming on the inner thigh.
Symptoms
While symptoms may vary in severity, most boils:
- are round, red, swollen bumps that grow gradually
- are tender and sensitive, sometimes even to air
- eventually discharge a whitish-colored pus made up of dead tissue and blood cells
- last for around 10 days
Boils may appear as a group or alone. Collectively, boils forming a group or cluster are called a carbuncle.
Boils, including the inner thigh, can occur on the body anywhere.
Causes and risk factors
Boils occur when the Staphyloccus auerus bacterium invades and colonizes the walls of a weakened or exposed hair follicle, causing infection.
The carriers of Staphyloccus auerus are some 10 to 20 percent of the population. Being a carrier means that on the surface of the skin of a person, the bacteria generally live.
The bacteria may be transmitted by skin-to – skin contact by carriers and individuals with boils. The bacteria, including towels and sheets, can also spread by contact with infected items. Infections arise in most individuals only when the protective barrier of the skin is broken or compromised by factors such as injury or friction.
Boils can be produced by anyone of any age. In areas of the body prone to chafing, particularly the inner thighs, they commonly occur.
It is understood that certain factors increase the risk of developing the disease.
Common risk factors for boils include:
- contact with someone infected with Staphyloccus aureus
- nicks or cuts in the skin
- living or working in a crowded area
- obesity
- immune conditions
- being over the age of 65
- diabetes
- poor hygiene
- animal scratches or bites
- smoking
- anemia
- iron deficiencies
- poor nutrition or diet
- lack of exercise
- prior use of antibiotics, especially multiple or improper usage in the past 6 months
- other skin infections or conditions, such as psoriasis and eczema
- long-term use of steroids or corticosteroids
- intravenous drug use
- extreme or chronic stress
A high risk of developing boils on the inner thigh may be due to particular factors. They include:
- wearing loose or ill-fitting clothing while exercising
- playing sports or doing exercises that cause chafing of the inner thighs, such as running, long-distance walking, hiking, or biking
- wearing dirty clothing, particularly when exercising or engaging in activities that involve inner-thigh friction or sweating
- walking or running in warm, humid climates
- shaving, waxing, and other means of hair removal that break the surface of the skin
When to see a doctor
Some boils require medical attention. Consult a doctor about boils that:
- appear on the face or upper neck
- do not rupture within about 10 days of forming
- will not fully drain
- do not fully heal within 1 to 3 weeks of rupturing
- are very painful and do not respond to over-the-counter anti-inflammatory or pain medications
- become more painful and swollen after rupturing
- seem to be spreading to new tissues
- feel soft and spongy
- leak pus from more than one location
- are larger than 5 millimeters
- include more than one head or point
- are clustered or blistering
- have drainage or fluid that is not white or clear
- are surrounded by a patch of skin that is painful, abnormal in color, or otherwise looks unhealthy
If a boil occurs at the same time as any of the following symptoms, a person should also see a doctor:
- nausea, vomiting, loss of appetite, or unexplained weight loss
- fever, chills, or other flu-like symptoms
- unexplained or abnormal bruising
Some people are at greater risk of boiling complications and are more likely to seek medical attention.
People with the following conditions should consider talking about their boils with a doctor:
- immune conditions
- diabetes
- people at risk for endocarditis, such as those with congenital or developed heart conditions
- anemia
- conditions that require management that weakens the immune system, such as chemotherapy
Treatments and home remedies
In most cases, with warm, soapy water, the first line of treatment is to clean the abscess and the surrounding skin. Stop touching, rubbing, or applying pressure to a boil that has just been cleaned.
There are ways of drawing the pus to the boil ‘s surface. This raises the abscess pressure, which makes the boil more likely to burst.
Home remedies
Diping a clean facecloth or towel in very hot water and gently holding it against the boil is one of the best ways to safely drain a boil at home.
Ideally, this compress should be as warm as possible without burning the skin. The towel or cloth should be left in place until it becomes cool or room temperature. For the boil to burst, it will also take several sessions. There are also hot compresses available in pharmacies.
When fighting boils at home, the following tips will help:
- Never force a boil to rupture by squeezing or piercing it.
- Keep a healing boil clean.
- Avoid touching, picking, or placing unnecessary pressure on a boil.
- Gently apply over-the-counter antiseptic and antibiotic creams and liquids.
- Cover a healing boil with gauze or a sterile bandage.
- Avoid activities that cause friction between the inner thighs.
- Take over-the-counter anti-inflammatories.
- Wash the hands with soap and water or use sanitizer after touching a boil.
- Wipe the surrounding skin daily for 1 week with a mixture of 70 percent isopropyl alcohol and 30 percent water.
- Encourage others in the household to practice similar precautions.
- Regularly replace personal hygiene products that can cause cuts and scrapes, particularly razor blades.
- For chronic or severe infections, wash every product that comes into contact with the body daily.
Medical treatments
To drain it, a doctor would need to cut it into a boil. If a boil is serious, very big, or if it won’t drain on its own, this might be required. In cases of chronic boils, incisions may also be required.
Oral antibiotics can also be administered by a doctor to clear up the infection. A physician may prescribe topical antibiotic creams or antibiotic nasal sprays if the boils are chronic or do not respond to oral medication alone.
How can boils be prevented?

The risk of developing boils can be minimized by the following tips:
- Use products designed to prevent chafing when playing sports or exercising.
- Modify these activities to lessen chafing.
- Wash the entire body with soap and water daily.
- Wash the hands regularly.
- Avoid picking the nose.
- Change and wash linens regularly.
- Wear properly fitting, clean clothing while exercising.
- Do not share towels, underwear, or sheets with other people, including family members.
- Eat a balanced, nutritious diet.
- Exercise regularly.
- Avoid or stop smoking.
- Maintain a healthy body weight.
- Consume a healthy amount of iron, through diet or supplements.
- Have a daily vitamin C intake of 1,000 micrograms.
- Never share personal hygiene products, especially those capable of breaking the skin’s surface, such as razors.
- Be careful not to cut the skin.
- Exfoliate skin that has had hair removed every few days.
Outlook
A common type of skin abscess is boils or furuncles. Within 10 days of formation, most rupture and after a boil drains, it appears to heal within 1 to 3 weeks.
Boils can lead to complications in some instances, including scarring and painful clustering deep beneath the surface of the skin. Such clusters of boils are known as carbuncles.
Severe boils or carbuncles, if left untreated, can result in life-threatening conditions. Systemic infections, which may compromise the bloodstream or the whole body, can involve these.
Speak to a doctor about boils that are very big, not healing on their own, or are complicated by additional symptoms or conditions.