The pancreas is an organ with a gland. It lies in the heart. It is part of the digestive system, producing insulin and other important enzymes and hormones which help break down food.
The pancreas has an endocrine function because it releases juices directly into the bloodstream, and because it releases juices into ducts it has an exocrine function.
The pancreas secretes toxins, or digestive juices, into the small intestine. There, food which has left the stomach begins to break down.
The pancreas also produces and secretes the hormone insulin into the blood stream, where it regulates the amount of glucose or sugar in the body. Insulin control problems can lead to diabetes.
Pancreatitis and pancreatic cancer are also possible health problems.
The pancreas secretes toxins, or digestive juices, into the small intestine. There, food which has left the stomach begins to break down.
The pancreas also produces and secretes the hormone insulin into the blood stream, where it regulates the amount of glucose or sugar in the body. Insulin control problems can lead to diabetes.
Pancreatitis and pancreatic cancer are also possible health problems.
Important facts about the pancreas
Below are a few key points about the pancreas. More detail is in the main article.
- The pancreas is a gland organ with a key role in digestion and glucose control.
- Problems related to the pancreas include diabetes and cancer.
- A healthful diet can contribute to maintaining a healthy pancreas.
Features
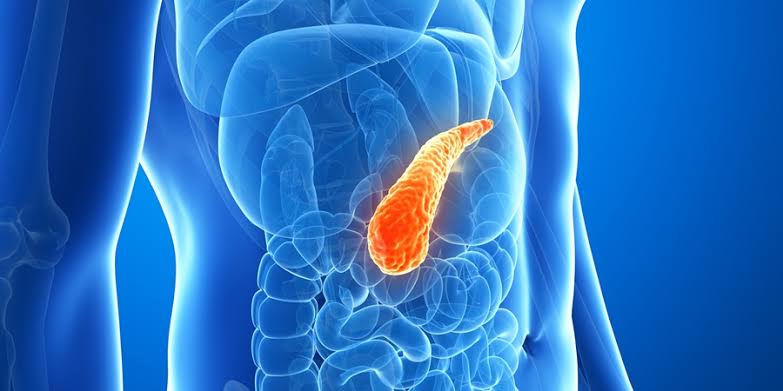
The pancreas is a six to eight inch long gland. It extends around the abdomen, horizontally.
The largest part lies on the right side of the abdomen, where the stomach is attached to the small intestine’s first part, the duodenum.
The partially digested food passes from the stomach into the small intestine at this stage, where it mixes with the pancreatic secretions.
The small section of the pancreas runs across the spleen to the left side of the abdomen.
A duct runs along the length of the pancreas, and several small branches of the glandular tissue join it. The end of this duct is connected to a similar duct from the liver that delivers bile to the duodenum.
Approximately 95 percent of the pancreas is exocrine. To assist with digestion it releases pancreatic enzymes. Every day a healthy pancreas produces about 2.2 pints (1 litre) of these enzymes.
The remaining 5 per cent is made up of hundreds of thousands of endocrine cells known as Langerhans islets. These grape-like clusters of cells produce significant hormones which regulate pancreatic secretions and control blood sugar.
Function
A healthy pancreas makes chemicals for digesting the food we eat.
The exocrine tissues secrete a clear , watery, alkaline juice with several enzymes in it. These break down the food into small molecules which the intestines can absorb.
The enzymes include:
- trypsin and chymotrypsin to digest proteins
- amylase to break down carbohydrates
- lipase, to break down fats into fatty acids and cholesterol
The Langerhans endocrine portion, or islets, secrete insulin and other hormones.
When blood sugar levels rise, pancreatic beta-cells release insulin.
Insulin:
- moves glucose from the blood into muscles and other tissues, for use as energy
- helps the liver absorb glucose, storing it as glycogen in case the body needs energy during stress or exercise
The pancreatic alpha cells release the hormone glucagon as blood sugar falls.
The glucagon helps the liver to break down glycogen into glucose.
Glucose then goes into the bloodstream, restoring blood sugar to normal levels.
Disorders
The pancreatic problems will affect the whole body.
For example, if the pancreas does not produce enough digestive enzymes, it will not absorb the food properly. This can cause diarrhea and weight loss.
The Langerhans islets have a duty to control blood glucose. Too little production of insulin will increase the risk of diabetes, and increase blood glucose levels.
Pancreatitis

Pancreatitis refers to an acute, or chronic, pancreatic inflammation. This has the ability to lead to secondary diabetes.
Inflammation may occur if a gallstone or tumor is blocking the main duct from the pancreas.
Pancreatic juices build up in the pancreas, causing pancreatic damage. The pancreas will start digesting itself.
Mumps, gallstones, trauma and the use of alcohol, steroids, and drugs can cause pancreatitis.
Acute pancreatitis is rare, but it needs immediate medical attention.
Symptoms include:
- intense abdominal pain, tenderness, and swelling
- nausea and vomiting
- fever
- muscle aches
Normally, immediate treatment is with fluids and pain relievers. For first, patients sometimes don’t want to eat, but if the pancreatitis is mild, they will actually eat relatively quickly again.
Where there has been a secondary infection, surgery may be necessary.
Chronic pancreatitis can develop if there is repeated occurrence of acute pancreatitis resulting in permanent damage.
Alcohol addiction is the most common cause and it often affects people in the middle ages.
Symptoms include:
- persistent pain in the upper abdomen and back
- weight loss
- diarrhea
- diabetes
- mild jaundice
Hereditary pancreatitis can occur if the pancreas or intestine has an inherited problem. An individual under the age of 30 can have recurrent, acute pancreatitis leading to a chronic condition.
It is a gradual condition which can result in permanent damage. The person may experience pain, diarrhea, diabetes or malnutrition. Treatment aims to control pain as a substitute for lost enzymes.
There is genetic testing for patients who may be at risk.
Pancreatic cancer
Cancer can develop in the pancreas. The exact cause is often unknown but often associated with smoking or heavy drinking.
Other risk factors include:
- diabetes
- chronic pancreatitis
- liver problems
- stomach infections
Symptoms include:
- pain in the upper abdomen as the tumor pushes against the nerves
- jaundice, a yellowing of the skin and eyes and darkening of the urine as the cancer interferes with the bile duct and the liver
- loss of appetite, nausea, and vomiting
- significant weight loss and weakness
- pale or gray stool, and excess fat in the stool
Symptoms can not occur until the cancer has entered its advanced stage. By then, successful treatment could be too late. Pancreatic Cancer prognosis tends to be poor.
Treatment typically requires surgery , radiation, chemotherapy or a mixture of these.
Palliative therapy will focus on relieving pain.
Pancreatic cancer is the fourth most common cause of cancer in men in the U.S., and the fifth among women. Per year more than 37,000 new cases are diagnosed.
Diabetes
Type 1 diabetes is an autoimmune condition. It happens when the immune system attacks and destroys the beta cells in the pancreas to prevent them from producing insulin any more. The precise cause is uncertain, but may be due to factors in genetics and the environment, including viruses.
Type 2 diabetes occurs when the body ‘s muscle, fat, and liver cells are unable to absorb glucose. The pancreas reacts by producing extra insulin, but can’t produce enough insulin in time. The body can’t control blood glucose levels any more.
Other problems that can occur include:
- Exocrine pancreatic insufficiency (EPI): The pancreas does not produce enough enzymes
- Pancreatic cysts: These can be removed by surgery if there is a risk of cancer
- Pancreatic fluid collections: Resulting from a range of conditions, this can lead to pain and fever
- Zollinger-Ellison syndrome: A tumor known as a gastinoma develops in the pancreas or duodenum
Maintaining a healthy pancreas
Following a balanced diet and avoiding smoking and drinking too much will help to keep the pancreas healthy.

The National Pancreatic Foundation recommend:
- consuming no more than 20 grams of fat a day
- avoiding alcohol
- drinking plenty of water to keep hydrated
According to the results of an animal study published in February 2017, a fasting diet may trigger the pancreas to regenerate itself which may help people with diabetes.
For a number of days a quick would involve consuming far fewer calories than usual.
The National Pancreatic Foundation is proposing a similar approach for people who suffer a pancreatic pain flare-up. They suggest taking a clear liquid diet, including grape juice, broth, gelatin, apple, and cranberry, for 1 to 2 days.
A fast can not provide all the necessary nutrients for wellbeing. People should ensure they consume healthy food after fasting to make up for missing nutrients.
Fasting should be discussed initially with a doctor.







